Occupational Violence Prevention: de-escalating the agitated, angry or defensive person
In previous Guardian Blogs, you would have read about reality-based training; train as you’re (hopefully not) going to fight! This blog will provide you a brief insight into some of our research, training and recommended techniques to de-escalate an aggressive, agitated, angry or defensive person.
Keep in mind, we focus on processes and techniques that keep you safe in the workplace and, as such, we recommend you seek assistance in dealing with a violent person. This needs to be approached with the assistance of police or security as attempted de-escalation in this setting is very challenging and heightens safety profiles for you and your workmates.
In Guardian’s contextualised training, you are provided an immersive education in well researched escalation pathways which demonstrates a predictable trajectory in mood from a normal state to someone being violent. At each level of mood differing engagement, techniques are recommended to enable safe de-escalation.
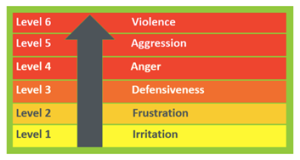
Multiple studies give clear evidenced support that communication, de-escalation and reality-based training all assist staff in developing a better understanding of their abilities and improving safety profiles in the workplace.
Violence prevention and management are important parts of inpatient psychiatric nursing because both patients and staff need to feel safe and secure. Positive appreciation of patients, emotional regulation and effective structure are recommended as part of a successful de-escalation process (Bjorkdahl, Hansebo and Palmstierna, 2012).
In a clinical setting, traditional methods of treating agitated patients, i.e. routine restraints and involuntary medication, have been replaced with a much greater emphasis on noncoercive approaches. Experienced practitioners have found that if such interventions are undertaken with genuine commitment, successful outcomes can occur far more often than previously thought possible. In the new paradigm, a 3-step approach is used. First, the patient is verbally engaged; then a collaborative relationship is established; and finally, the patient is verbally de-escalated out of the agitated state (Richmond, et al., 2012).

In Guardian’s reality-based training, you will receive valuable training on overcoming barriers in communication and how best to improve your success in de-escalation. Some of the main points to consider are:
- remove distractions and utilise a low sensory, more private area;
- maintain a safe distance for safety and personal space for the patient;
- use neutral tone and body language as these are key in successful communication;
- adjust communication structure and style to validate and empathise in a non-judgemental manner; and
- set boundaries and avoid challenging questions.
Want to know more? Check out Guardian’s online courses and start learning today!
Or for further information on face-to-face or virtual courses, please touch base using the following email address: [email protected]
References:
Richmond, J., Berlin, J., Fishkind, A., Holloman, G., Zeller, S., Wilson, M., Rifai, M.A. and Ng, A. (2012). Verbal De-escalation of the Agitated Patient: Consensus Statement of the American Association for Emergency Psychiatry Project BETA De-escalation Workgroup. Western Journal of Emergency Medicine, [online] 13(1), pp.17–25. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3298202/.
BJÖRKDAHL, A., HANSEBO, G. and PALMSTIERNA, T. (2012). The influence of staff training on the violence prevention and management climate in psychiatric inpatient units. Journal of Psychiatric and Mental Health Nursing, 20(5), pp.396–404.